Cornea Transplantation
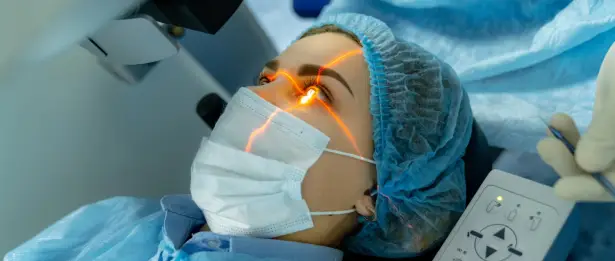
What is Cornea Transplantation?
Cornea transplant is the replacement of corneal tissue (the transparent tissue at the front of the eye). Since this tissue also has a lens feature, not only its transparency but also its optical properties are very important for the eye to see clearly. Corneal transplantation is required when vision is negatively affected due to edema (blurring), deformation, and spots as a result of various diseases.
How is Cornea Transplant Done?
It is performed by two different methods: penetrating (replacement of all corneal layers) and lamellar (replacement of only the diseased layer). In recent years, lamellar keratoplasty has been increasingly applied. Because if the patient's own tissue is intact, protecting that tissue is considered the main goal. Lamellar keratoplasty can be a replacement of the front corneal tissue (anterior lamellar) or a replacement of the back corneal tissue (posterior lamellar).
Is Laser Used in Cornea Transplantation?
Laser use has also increased in recent years. Although it is not very common yet, surgery can be performed using laser in appropriate cases. Femtosecond laser is used in corneal transplants. It is especially advantageous in eyes suitable for use in anterior lamellar keratoplasty.
What is Sutureless Cornea Transplantation?
In most diseases that require corneal transplantation, only a certain layer of the cornea is damaged. In seamless corneal transplantation, only the damaged inner cell layer is replaced. The endothelial cell layer is the innermost layer of the cornea. The most important function of these cells is to keep the cornea transparent for clear vision. Corneal edema develops in some genetic diseases and after eye surgeries in which endothelial cells are damaged. The patient group for which seamless corneal transplantation is most commonly performed is patients who develop corneal edema following unsuccessful cataract surgery.
What is the Difference of Seamless Cornea Transplantation?
All corneal transplant surgeries are performed under sterile conditions with the help of an operating microscope. Apart from the corneal tissue, the equipment and technology to be used in the surgery vary depending on the transplantation technique. In full-thickness corneal transplants, after the damaged or cloudy corneal tissue is removed, the donor corneal tissue is fixed to the eye with stitches. These stitches are removed one by one 6 months after the surgery, in parallel with the wound healing. Although vision is better immediately after the surgery than before, the best vision is achieved 6 months to 1 year later, after the stitches that create astigmatism are removed and appropriate glasses or contact lenses are prescribed.
Some stitches may be permanent, depending on the condition of the eye. In seamless corneal transplantation, the corneal tissue taken from the donor is separated into layers with devices called microkeratomes. The damaged endothelial layer is removed from the patient and the donor cornea is placed into the eye through a 3.5 mm incision. A small air bubble injected into the eye is also used to fix the graft. Only stitches are placed at the surgical site, to be removed after 1 week. A few days after the surgery, vision reaches the target level.
Where to Find Corneal Tissue for Transplantation?
Cornea is obtained from cornea banks. This is a necessity both from a legal and health perspective; because when transplanting tissue, it is possible to transplant various diseases and risks. To prevent this, this procedure must be followed.
Why is Cornea Transplant Done?
Cornea transplantation can be performed for four purposes. The first and most important of these is optical reasons. The second and less common situation is the disruption of the integrity of the eye, also called tectonics. Cornea transplantation is done thirdly to treat infections. The fourth reason is to provide an aesthetic appearance to the dark gray layer formed by the cornea in eyes with very low or no vision.
What Happens If Keratoconus Is Untreated?
Most of the time, corneal transplantation is required in cases of hereditary, infectious or post-traumatic diseases. These diseases include keratoconus and pallucid marginal degeneration keratoglobus; It causes signs of corneal convexity, thinning, myopia and increased astigmatism. Among this group of diseases, keratoconus is especially important as it occurs much more frequently and at an earlier age. It usually occurs between the ages of 10-15 and is progressive. If left untreated, a significant portion of patients will need a corneal transplant.
There are many diseases that fall into the corneal dystrophies group, and this condition causes opacification between the various layers of the cornea. In addition, keratitis corneal infections cause the corneal tissue to be susceptible to infections due to bacterial, viral or fungal diseases. For this reason, infections need to be treated quickly and effectively, otherwise it may cause a decrease in vision or even loss of the eye.
What Should Be Considered After Cornea Transplant Surgery?
Follow-up after surgery is very important. If the patient who underwent surgery lives abroad, they need to contact a doctor who they are sure can follow the patient. Patients should be examined by a doctor at regular intervals and It needs to be used regularly. Especially patients who have undergone a full-thickness transplant should be informed about the rejection reaction. If there are symptoms such as mild pain and redness in the eye or blurred vision, the patient should definitely consult a doctor.
How is Astigmatism Treated After Cornea Transplantation?
Artificial cornea applications may be considered in eyes where corneal transplantation is not suitable or has failed, and postoperative surgery is as important as surgery. In some types of surgeries, there is a possibility that the tissue may be rejected by the body and the patient must use medication very carefully. It is essential that the patient establishes a very good connection with his doctor. Because if the body gets into a position to reject that tissue, it must be stopped immediately. The patient should be monitored for at least 6 months or longer depending on the situation. After corneal transplantation, there may be significant increases in eye size, especially in astigmatism. These can be corrected by methods such as laser, intracorneal ring or intraocular lens after the tissue has settled.
* Contents of this page is for informational purposes only. Please consult your doctor for diagnosis and treatment. The content of this page does not include information on medicinal health care at Liv Hospital









